#Current Affairs
Save Rohingya: A Physician’s Journal, Part 2
Published
By
Guests
By Tasneem Hoque, MD
This is a continuation of Save Rohingya: A Physician’s Journal, Part 1
January 16, 2018: Day 8, Thaingkhali Camp Block E4
It was quite a busy day as our team saw 612 patients in just about 5 hours. We went deep into Block E, over steep hills, near the back rim of the camp, a little over a mile away from the “main center” of Thaingkhali where our van and ambulance were parked.
Keep supporting MuslimMatters for the sake of Allah
Alhamdulillah, we're at over 850 supporters. Help us get to 900 supporters this month. All it takes is a small gift from a reader like you to keep us going, for just $2 / month.
The Prophet (SAW) has taught us the best of deeds are those that done consistently, even if they are small. Click here to support MuslimMatters with a monthly donation of $2 per month. Set it and collect blessings from Allah (swt) for the khayr you're supporting without thinking about it.
When ill, most of these patients are treated by “Burmese” doctors – local Rohingya homeopathic medicine men with no formal medical training. In Myanmar, the Rohingya were not allowed to pursue education beyond the 10th grade. Furthermore, those who completed 10th grade were not allowed to sit for the formal O and A level exams necessary to pursue any higher education. The local imam for the region today informed us that no mobile clinic had ever visited this area – ours was the first and the community was very excited.
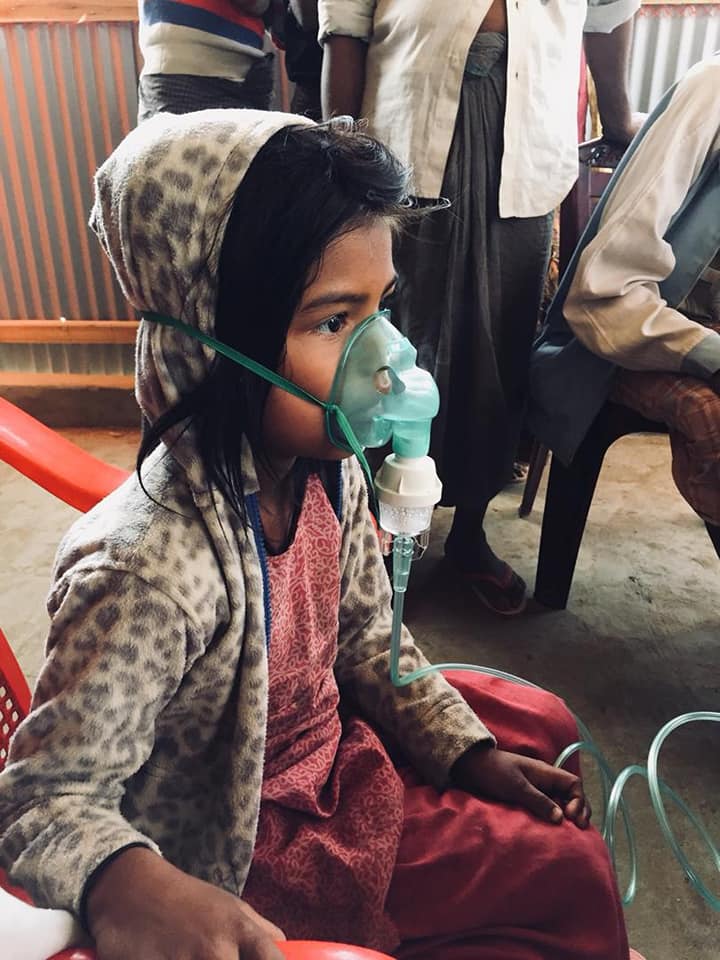
Young girl using nebulizer
It was a special day (they all have been) because we were able to use a portable nebulizer on our younger patients. One of the biggest difficulties we encountered in the days prior was the inability to provide simple asthma management. Albuterol inhalers were present in our mobile pharmacy, however, we did not have spacers. As a result, we had to get imaginative about creating spacers for patients, using cups or bottles. Inhaler compliance and proper use remained lingering concerns. Plus, inhalers were really only an option for adults and older children. Young children and infants with shortness of breath, cough, or wheezing could not use an inhaler at all. To address this, IMANA purchased and sent a small portable nebulizer that could be used to treat these children and provide instantaneous relief.
Out of the 612 patients seen, we had only 3 referrals to the Malaysian Field Hospital. In the last few days, we’ve had many patients whose ailments warranted urgent care but in these dire settings, unless it’s an emergency and potentially life-threatening, the various NGO field hospitals do not have the manpower or resources to manage the less acute cases. It’s a shocking and startling reminder of just how different our worlds are. Luckily, none of the children I saw today were acutely ill. Rather, this group of children was remarkably more social, less inhibited, and more engaged than most of the children I had seen in the past week. I hope the photos convey the innocence of their young lives.
January 17, 2018: Day 9, Thaingkhali Camp, Block D11
Each day has been full of surprises – sometimes they are sweet, mostly they are demoralizing. Today was especially memorable for its unexpected moments. Fair warning: the following story and photo are graphic so if you have a weak stomach, I would skip the next section and the picture.
Impossible Choices
The very first patient of the day was a 7-year-old girl named Purwas Begum. She was found sitting on the ground just inside the doorway of the clinic hut, hiding beneath a dusty sheet of tarp, whimpering in pain. Once found, she refused to speak, even to the translator. Her father, an elderly man (though understandably, all the Rohingya appear older than their reported ages) appeared within a few minutes, picked her up, and carried her to the table.
I couldn’t understand why a 7-year-old needed to be carried until her father exposed his daughter’s left foot, revealing a large wound covering the length of the inner left foot, starting at the left big toe and extending to just beneath the inner left ankle. Pus was oozing from beneath a large scab that was floating atop the wound. She would barely allow me to examine the injury, but the big toe was already turning purple in color. She couldn’t move the toe or the ankle, and there was a small portion where bone was exposed. She was having intermittent fevers. The father informed me that the foot was run-over by a jeep 3 weeks prior. He had taken her to the “Burmese” doctor who gave her an injection for 3000 taka. With no disrespect to the centuries-old practices of homeopathic medicine, these Burmese doctors are Rohingya medicine men from Myanmar with no formal medical education. The father couldn’t tell me what the injection was. When asked how he secured 3000 taka (~$35 USD, but a hefty amount in Bangladesh) he said the local imam had collected it.
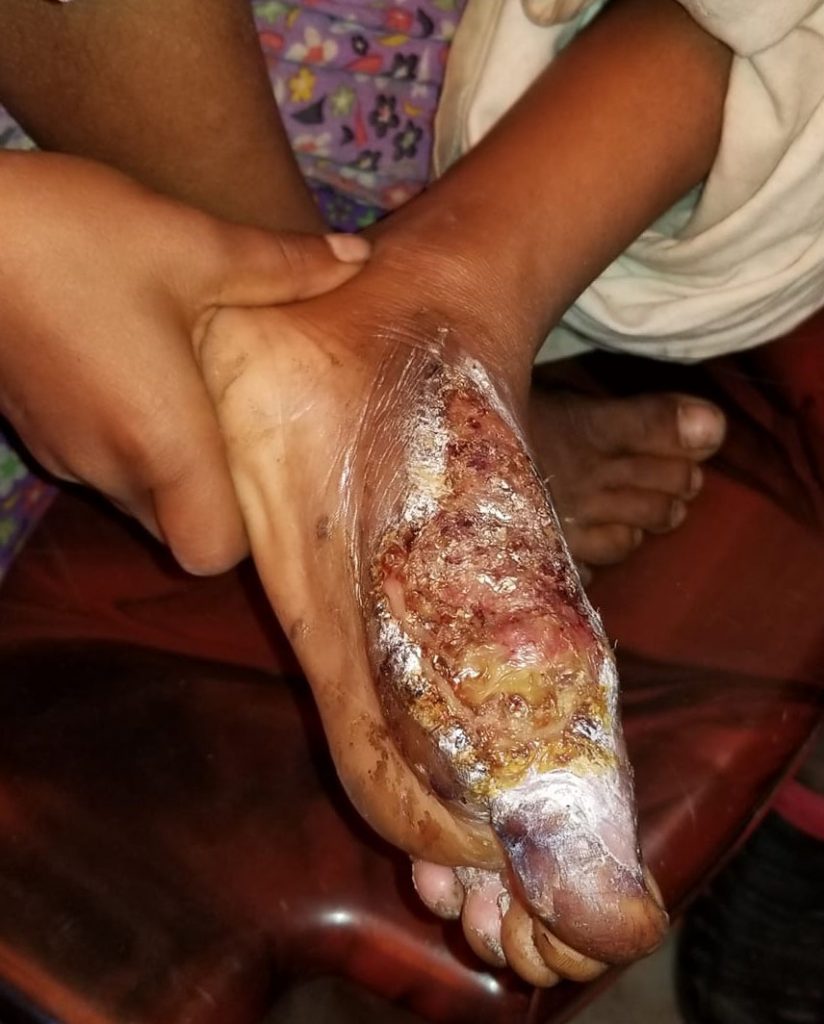
Purwas Begum’s left foot
I told the father that his daughter’s foot needed serious medical attention – that I’d like to send them by ambulance to the Malaysian Field Hospital so she may receive IV antibiotics and have the wound cleaned out, likely under sedation, to try to salvage as much of the foot as possible and maybe regain some mobility. He refused to go despite my pleas, stating that if he went to the hospital the Burmese doctor would no longer treat his daughter.
Can you imagine? How many times can one person beg? My brain was firing like crazy trying to stay rational while attempting to calmly convey to the father my concerns for gangrene, possible auto-amputation (at least of that big toe) and, of course, infection that could take her life. I was angry, profoundly saddened, and so worried, but had no option but to comply with the father’s wishes. I gave him a prescription for oral antibiotics (which would do nothing), pain medication, and some clean bandages. I also gave him the number to our mobile clinic’s site organizer in case he changed his mind — that way he could contact us and we would bring her to the hospital.
Impossible choices. Unfathomable conditions. Such is the grim reality of their existence.
A Morning Star
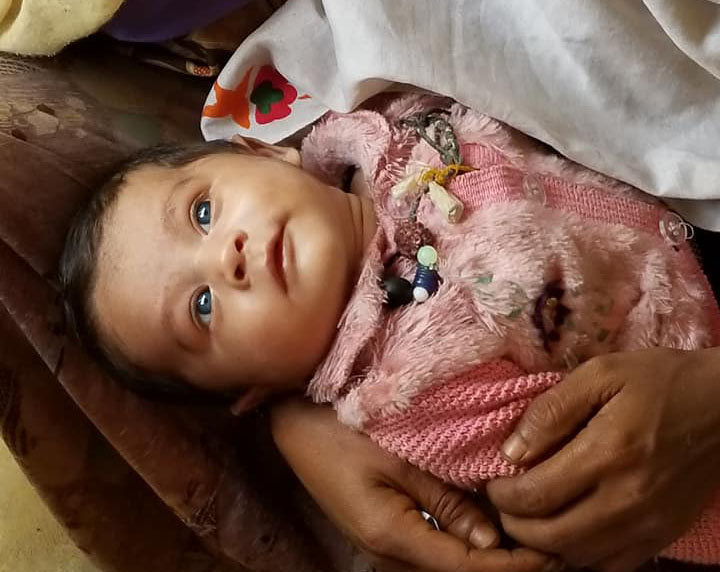
Mr. Tariq Alam
Two patients later, a young woman sat down next to me and presented her infant son. I recognized him immediately as the baby boy with piercing blue eyes whose mother my colleagues had been talking to outside the clinic door. I asked for his name, age, and chief complaint. She responded that he was 1-month-old and she just wanted him checked by a doctor to make sure he was ok, but hesitated to give me a name. When I asked again, she sheepishly grinned and admitted he wasn’t given one yet. As I started to ask her for her name, she interrupted me and mumbled something in the Rohingya dialect (many of their words are quite similar to Bengali but beyond simple phrases, I couldn’t understand what they were saying). I asked the translator what she said, to which he responded, “She wants you to name her son.”
I was taken aback and replied, “Surely, you don’t want me, a complete stranger, to name your first child, instead of the grandparent?”
She shyly smiled again and said she decided that morning, while waiting outside, that she wanted her son to be named by the foreign woman doctor when she heard I was Muslim. She hoped it would mean that her son’s life would be better than this place and that he, too, would grow up to be a doctor.
I honestly didn’t want to acquiesce because it felt like an enormous responsibility and, truthfully, I didn’t think I deserved such an honor. Besides, what if he hated the name he was given? She asked again and my colleague sitting next to me said, “You should do it. Pick a name.”
And so I did. I gave him the first name Tariq (“morning star” in Arabic) for his celestial baby blue eyes, followed by his father’s name, Alam. Tariq Alam. I don’t know if I’ll ever be blessed to have children of my own, but I will be forever grateful to Tariq’s mother for gifting me this unforgettable moment.
The One who cares for an Orphan
As the day progressed, my colleagues and I saw numerous patients – 502 to be exact. The area was yet again a region that had not been reached by other mobile clinics. The lines were wrapped around the hut. The women at one point were on the verge of stampede to get into the hut’s doorway. A young woman and her toddler were knocked to the ground. We had to shut the door and post “guards” to control the flow of patients into the room.

Mother with her adopted 3-year-old
A colleague evaluated a 3-year-old girl who was clearly developmentally delayed, with an underdeveloped head and low muscle tone. She was also deaf and mute. As it turned out, the woman with her was not her mother. This woman told us that she found the little girl on the roadside as she was escaping her own burning home, one of the many in her village that were set afire by the Myanmar military. She found the child crying next to the slaughtered bodies of two people she presumed were the young girl’s parents. She carried the child the entire way to safety in Bangladesh. She told our team she had no children of her own and planned to raise this girl rather than place her in an orphanage. She had come to the clinic with concerns about the child’s delays and refused to believe that the little girl was beyond help, contrary to what others in the village had said. She told my colleague she would never give up on her.
There is a hadith narrated by the Prophet Muhammad 
“The one who cares for an orphan and myself will be together in Paradise like this,” and he held his two fingers together to illustrate. (Ṣaḥīḥ al-Bukhārī)
I can only imagine the immense reward this woman will be getting when she so lovingly took care of this child immediately after losing everything herself.
The stories that lie behind the tired eyes of these people are enough to compile volumes, an encyclopedia of suffering. They are victims of life’s cruelest plots. Violence still abounds. Women and children are at risk of kidnap and rape in the night, as they go to use the latrines. Even within the confines of these vast camps, it can hardly be considered sanctuary. Yet, the Rohingya consistently display the qualities of generosity, patience, and gratitude to a degree I have not witnessed in many others.
January 18, 2018: Day 10, Thaingkhali Camp, Block D9
My last day with the mobile clinic, my last day with the Rohingya.
When I signed up for this mission in early December 2017, I never could have imagined just how deeply attached I would become to the people, their stories, and their plight. It’s as if my very DNA has mutated.

Sunrise in Cox’s Bazaar

Walking to work!
I awoke to a beautiful morning adhan for Fajr. You don’t need to be Muslim to appreciate the hypnotic, lilting cadence of the call to prayer, and this particular morning’s adhan sounded near-ethereal. A glowing, salmony, golden-pink sunrise guided the morning’s 3-mile run along the beach. On any other day, even the car ride to the day’s camp site would have ruined the morning’s zen. A truck lodged itself into a ditch on the narrow dirt road costing us a precious hour. At that point, our team of volunteers (doctors & locals) all agreed unanimously to get out of the car, gather up the medication boxes, and trek to our site, leaving our driver to move the car when the jam was relieved. Some of the group hopped onto traditional rickshaws, some others jumped into tuk-tuks. I chose to walk. I wanted to feel the earth beneath my feet.
It was a brilliantly sunny day. In the many days prior, a dense blanket of fog descended to the ground, lifting a little as the day progressed but impairing visibility throughout each day. Upon reaching the clinic site, the patients were already lined up around the large hut waiting to be seen – women and children on one side, men on the other. I tried to work as fast as I could – to see as many as I could. Being the only pediatric physician and the only female in our medical group that day, there were over a hundred women and children lined up to be seen by me. I wanted to stretch the hours, second by second, see each patient, hear their stories, and not lose a single moment. We had already lost so much time due to the traffic jam and I hated even more that I had to leave around noon to catch my flight back to Dhaka that evening.
Maladies of the Soul

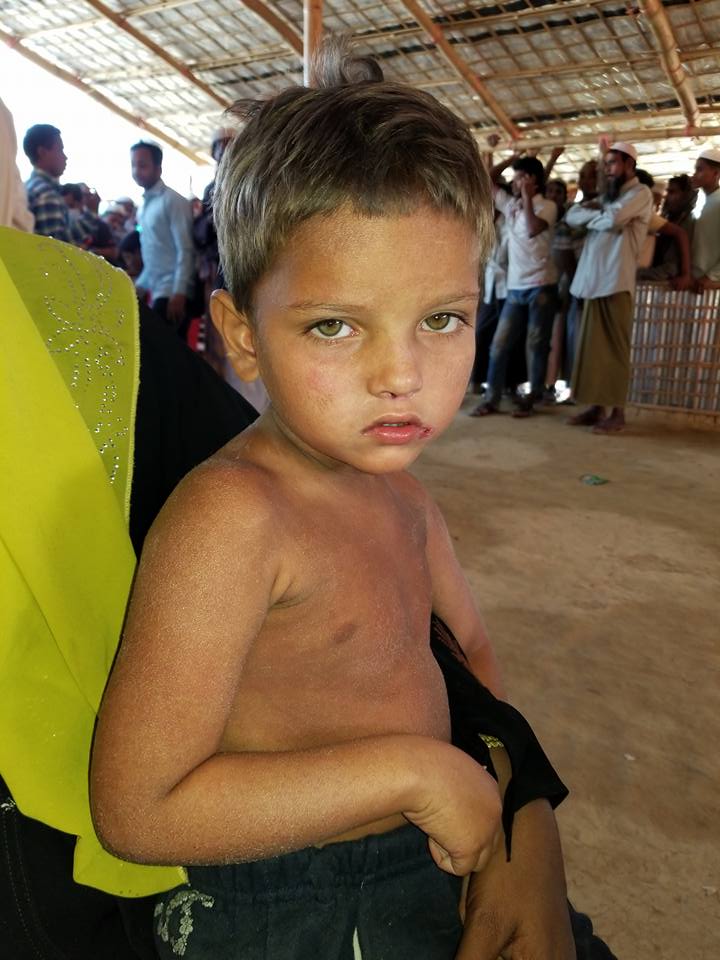
Mr. Arman
A short while later, a little 3-year-old boy, Arman, who I had diagnosed the previous day with scarlet fever, showed up for a repeat check-up. He was brought by his neighbor because his own mother had just given birth two days before. This woman had kept the young boy in her hut while he was ill so he wouldn’t affect the mother or the new baby. As miserable as Arman was just the day before, within 24 hours of starting antibiotics his fever was gone and the sandpaper rash was much improved. He even smiled a few times (though not for the camera).
One of the last patients I saw was an infant girl named Hasina, believed to be about 45-days-old but the mother couldn’t be sure. She weighed less than 1.5 kg. The mother said her own milk supply was low, the baby wouldn’t latch, and that she was spoon-feeding the baby powdered milk mixed with water. She was now worried because the baby wasn’t making urine as much, and was becoming too skinny. The mother was young, only 17-years-old, and was accompanied by her mother-in-law. My thoughts kept drifting back to the idea that if we could just get these young mothers lactation consultants, so many of the babies would do so much better! Luckily, unlike some prior experiences, this family was willing to have the baby admitted to the hospital (thank goodness!) and I later had the honor of riding in the ambulance with them as I took my final leave out of the camp.
By 12:15 pm, as I was being reminded of the rapidly dwindling time I suddenly froze, staring dejectedly at the line of women and children waiting to be seen at my end of the table. I felt dumbfounded and defeated. How could I just walk away and leave? One of the team doctors broke my trance and gently assured me that all of these people would be seen. As I attempted to say my goodbyes, I became tongue-tied and teary-eyed. I was overtaken by a profound wave of sadness. I would never see or know what happened to all these people whose faces were branded into my memory. They had no cell phones, no addresses. In medicine, we aim for relief of illness, alleviation of pain and suffering, prevention and cures for diseases, all in the hopes of returning the infirm to their health and livelihood.
I couldn’t help but think, what is going to happen to the nearly 700,000 souls that live in these cramped, dusty, dirty, tarpaulin huts with no access to steady food resources, no income, no reliable healthcare access, no education? I get to return to a world of flushable toilets, electricity, computers, excessive food production, and woefully excessive waste. I go back to a world of luxury. What is their future? Is there one? Or am I looking upon an entire generation lost? How to reconcile this dichotomy?

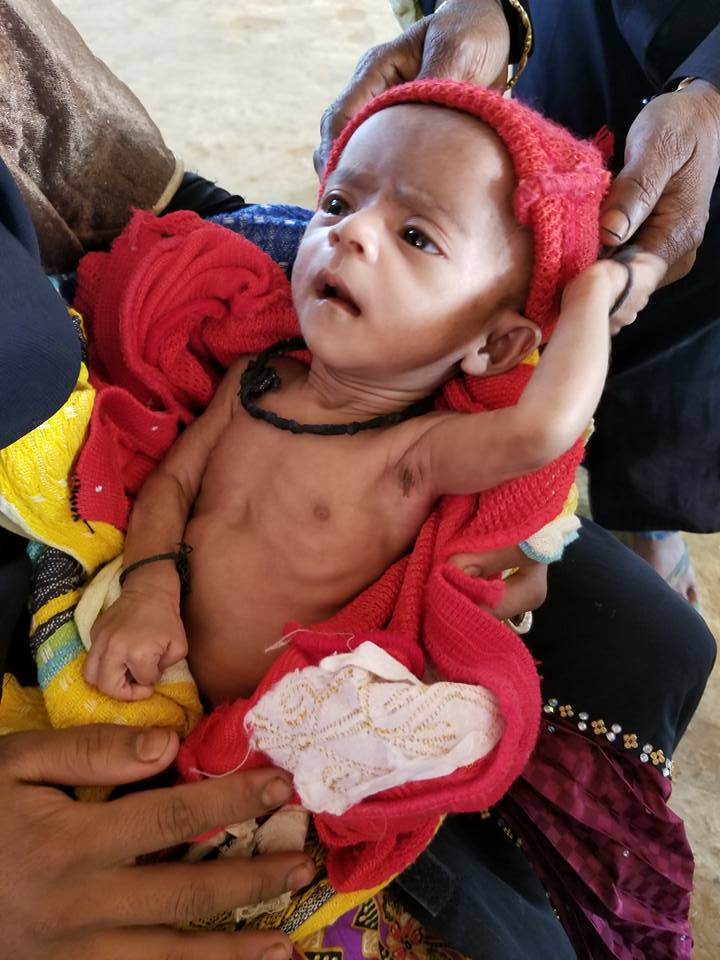
Miss Hasina
During the ambulance ride with baby Hasina, her mom, and her Dadi (paternal grandmother), I fought through my tears and asked the Dadi if she would be willing to share her family’s story with me. It was a relatively happy one compared to the others. She said she has three sons, all of whom were married, baby Hasina’s father being the youngest of her sons. She lost her own husband in 2012, during the last round of violence against the Rohingya. He, too, had gone out to collect items from the nearest town but never returned. Of all her grandchildren, she was most excited for baby Hasina because she was the first girl of the current generation. She told me she felt immediately connected to the little girl since her own daughter had been killed, and thought this was God’s way of returning her daughter’s spirit to her. After dropping them off at the hospital, the Dadi grasped my hand and repeated, “Dua, dua” (prayers for you).
I am haunted, uplifted, humbled, and re-invigorated by these people. They have taught me more about life in 10 days than my nearly 4 decades of age.
These two weeks with the Rohingya were a welcome and much-needed reminder of why I became a doctor. I am so grateful to IMANA for launching these missions and creating an opportunity to provide essential medical care to an impoverished people. Our team treated over 6,200 patients in my two weeks, and IMANA has evaluated 18,000+ patients to date, purchased a second ambulance, and extended their missions into April.
What can you do?
Monetary contributions and volunteers are always needed by IMANA and the numerous other NGOs listed below, that are on the ground in Bangladesh. In addition, Burma Task Force (BTF) is a coalition of 19 US and Canadian Muslim organizations, under the parent organization, Justice For All, a 501(c)(3) nonprofit, dedicated to advocating for the Rohingya and ending the genocide in Burma. BTF encourages you to contact your senators and representatives and urge them to pass the Bill To Promote Democracy and Human Rights in Burma and the Burma Act of 2017. For more information and a specific action plan visit Burma Task Force.
NGOs on the ground in Bangladesh:
Bangladesh Rural Advancement Committee (BRAC)
International Rescue Committee
Tasneem Hoque, MD was inspired to return to her ancestral home of Bangladesh out of a deep desire to help with the devastating plight of the Rohingya people. Tasneem completed her residency in pediatrics and her fellowship in pediatric cardiology at Columbia University Medical Center in New York City. Providing care and service to people is her passion, but she is also committed to serving her community through various charity works, humanitarian causes, and by inspiring youth to achieve their dreams. She is a founding board member for the Khan Foundation, a 501(c)(3) nonprofit organization geared at improving college access to low-income and underprivileged youth in New York City.
Keep supporting MuslimMatters for the sake of Allah
Alhamdulillah, we're at over 850 supporters. Help us get to 900 supporters this month. All it takes is a small gift from a reader like you to keep us going, for just $2 / month.
The Prophet (SAW) has taught us the best of deeds are those that done consistently, even if they are small. Click here to support MuslimMatters with a monthly donation of $2 per month. Set it and collect blessings from Allah (swt) for the khayr you're supporting without thinking about it.

Protecting Our Children As They Learn Quran Online: A Guide For Parents

The MM Recap: Our Most Popular Dhul Hijjah And Hajj Articles [2026 Edition]

The Spiritual Weight Of Dhul Hijjah And The Sincerity Of Sacrifice

Far Away [Part 13] – Brotherhood Under A Bridge

Not Everyone Goes To Hajj…But Everyone Is Called: Gaza, Gratitude, And Dhul Hijjah

Op-Ed: Javed Ghamidi And The Theology Of Managed Defeat

Why Liberation Is Sexual(ized) – The Forces Driving The Unquenchable Thirst To Emancipate Muslim Women

[Podcast] Can the Golden Age of Islam Save Us? | Sh Abdullah Mullanee

Daughter Of Which Nation? The Persecution Of Asiya Andrabi And India’s Crackdown On Muslims

Beyond Representation: Reclaiming Spiritual Storytelling For Muslim Children

Coming Full Circle: Who Are You Now? | Night 30 with the Qur’an

Running Away From Who We Are | Night 29 with the Qur’an

Building From the Ground Up: Week 4 Recap | Night 28 with the Qur’an

The Muslim You Are Becoming | Night 27 with the Qur’an

What Will You Leave Behind? Legacy in Islam | Night 25 with the Qur’an
Trending
-
#Current Affairs3 weeks ago
Op-Ed: Javed Ghamidi And The Theology Of Managed Defeat
-
#Culture1 month ago
The Boycott: A Simulation Of The Valley Of Shib Abi Talib
-
#Current Affairs3 weeks ago
Why Liberation Is Sexual(ized) – The Forces Driving The Unquenchable Thirst To Emancipate Muslim Women
-
#Culture1 month ago
Muslim Capitalism And The Rise of Tech And VC Culture: Are We Going Down The Technological Lizard Hole?














Taoheedah
March 22, 2018 at 2:28 PM
So heart breaking and so uplifting at the same time reading about what doctors and volunteers like Dr. Tasneem are doing. May Almighty Allah accept it all from you as ibadah and may He alleviate the sufferings of the Rohingya people. Ameen. Jazakumllahu khayran to MM for publishing this.