#Current Affairs
Save Rohingya: A Physician’s Journal, Part 1
Published
By
Guests
By Tasneem Hoque, MD
The Islamic Medical Association of North America (IMANA) began medical relief missions to the Rohingya refugee camps in Bangladesh in late December 2017. Missions are currently running through the end of April 2018 with the intention, insh’Allah, to extend missions to the end of May and beyond, if financially possible. IMANA volunteer physicians conduct mobile clinics 1-2 weeks at a time in a joint collaboration with the Islamic Medical Association of Malaysia Response and Relief Team (IMARET) and the Charitable Society of Bangladeshi Doctors (CSBD). The goal of the mobile clinic is to reach the farthest areas of each section of the camps since the farther the refugees are from the main center, the less likely they are to have contact with the locals and seek or receive medical care. Here is the account of Dr. Tasneem Hoque, a pediatric cardiologist from New York City, who spent two weeks caring for the Rohingya in mid-January 2018.
January 9, 2018: Day 1, Balukhali Camp Block K9
Keep supporting MuslimMatters for the sake of Allah
Alhamdulillah, we're at over 850 supporters. Help us get to 900 supporters this month. All it takes is a small gift from a reader like you to keep us going, for just $2 / month.
The Prophet (SAW) has taught us the best of deeds are those that done consistently, even if they are small. Click here to support MuslimMatters with a monthly donation of $2 per month. Set it and collect blessings from Allah (swt) for the khayr you're supporting without thinking about it.
First day completed. The conditions here are not fit for animals, let alone humans. I saw makeshift huts jammed onto rough, muddy hillsides, water wells contaminated by nearby latrines, rapidly-spreading and easily communicable diseases given the degree of overcrowding, poor sanitation, and limited access to healthcare. It was heartbreaking to witness and today was only my first day.

Patient with goiter
Our team saw around 370 patients in the mobile clinic today, more than half of whom were children. A few cases stood out for me. There was a 15-year-old girl with progressive loss of vision over the last few years and now nearly blind, a 30-year-old woman with massive goiter (a swelling of the neck resulting from enlargement of the thyroid gland) and complaints of malaise who lost everyone in her family to military violence in Myanmar, and a 75-year-old woman who escaped Myanmar with only one surviving sister after her husband went missing, her children and the rest of her family shot and killed. The last two patients of the day were seen after clinic had ended: the 3-year-old boy with a large herpes infection of the right lip and cheek that was further complicated by a bacterial infection, and the 4-year-old boy with a cough who was in respiratory distress.
Everything that has been said about these camps is horrifyingly real.
January 10-11, 2018: Days 2-3, Thaingkhali Camp Block A
A different camp, “slightly” less crowded but the stories are the same – tales from survivors of family members who were tortured and killed in front of their own eyes, gunshot wound injuries that have left irreparable soft tissue and bony damage, machete attacks that have since “healed” but left severely limited mobility in the affected limb, infants with inflammations or lung infections, and diphtheria outbreaks.
The biggest complaints are far less dramatic though – stomach ulcers, anemia, fatigue, coughs, colds, body aches, weakness, malnutrition, lightheadedness, loss of appetite, and pregnancy. I did my first obstetric ultrasound since medical school. The cardiologist in me snuck in a quick scan of the fetal heart to rule out congenital heart disease! This has certainly been a crash course in primary care medicine for me, and I hope I did right by these patients.

Teaching kids hopscotch

Impromptu soccer game
There was a bit of levity to the day too! I introduced the kids to hopscotch and tic-tac-toe (drawn in the dirt). The male doctors in our team snuck in a game of volleyball and also a bit of soccer with the camp inhabitants. I somehow managed to acquire an entourage on my way out of the camp. An 80-year-old man got a bar of soap and said he felt like the luckiest man alive, and a 95-year-old woman kissed my forehead on her way out of the clinic.
January 12-13, 2018: Days 4-5, Thaingkhali Camp Blocks B & C
Brace yourself because this entry is very long.

A great majority of the Rohingya people we are seeing have complaints consisting of body aches, dizziness, weakness, and insomnia that rarely amount to any actual disease but are likely signs of depression, post-traumatic stress, and anxiety. However, two young babies yesterday highlighted, in neon blazing, glaring lights, the harsh realities of the Rohingya world. Despite seeing over 470 patients on each of the two days, these two young infants simultaneously captured my heart and crushed it.
Miss Rashida
“Though she be but little, she is fierce.” – Will Shakespeare

Miss Rashida
Miss Rashida was a 38-day-old infant with severe malnutrition. She weighed, at best, 1 kg (2.2 lbs). The mother reported that she carried the child for 9 months, but she looked as if she was a 28-week-old premature infant. Rashida was severely dehydrated with sunken eyes and barely flinched when I touched her. The mother reported that her breast milk supply was much lower lately, and the infant was not interested in suckling. I told the mother that I wanted to send her and the infant by ambulance to the Malaysian Field Hospital, where the infant could get rehydrated and started on a refeeding protocol. Otherwise, the infant would surely die.
She looked at me solemnly, and quietly refused.
She couldn’t go because she would want her own mother to be there with her. However, both she and her mother needed to be home because they were awaiting someone later that day who would register them, the child, as well as their location so that the family could receive rations from distribution centers (without registration, you are not eligible). Her husband didn’t make it out of Myanmar. He had been killed before the infant was born.
Profound sadness washed over me. I begged the mother, with the help of one of the translators, to allow us to transport them, to give the baby a fighting chance. I couldn’t even be angry at her distrust of authority. Honestly, why wouldn’t she? After 30 minutes of pleading, she finally understood the gravity of the situation and agreed.
Mr. Mahmud
The second child, Mahmud, was a 1 ½-year-old boy whose father reported that he was born weak and had always had a little trouble breathing. However, in the last week, the child had daily fevers and was “sucking in” at the chest and throat with each of his breaths, was very cranky, and weaker than usual. He had a fever and was breathing fast, at 50 breaths per minute. I told the father that I thought his son had pneumonia (he didn’t know what that was) and needed to be transferred to the field hospital where he could get full treatment and antibiotics.
He gave me a troubled and sad look, and said he couldn’t go.
His wife should be the one to go with the child, but she couldn’t because they had two other small children. He wouldn’t be able to care for them if she wasn’t there, and the family didn’t want to separate.
I looked at the father and then his son and started to cry. For the second time that day, I begged. I begged the father to let us treat his son, to allow him the chance to breathe. I told him the boy could die if left untreated, that they would be safe in the hospital, that they would not be returned to Myanmar, that we would make sure that if his son was admitted our team would bring his wife and family to the hospital to be together. He finally agreed, though reluctantly…

Mr. Mahmud
I was unable to sleep that night. I was so unraveled. I took an oath to serve and heal yet I was powerless yesterday. Neither an American medical school education, nor an Ivy League residency and fellowship training was of any use to me. Mahmud’s sweet yet sad gaze penetrated my core. He hadn’t taken his eyes off me… a still, sad, questioning stare silently screaming, “What are you going to do to me?”
How is it possible that we live on the same planet? People like me, living in excessive abundance, and people like them, barely living, without even the simplest of necessities. To be forced with choosing between one child and the livelihood of the rest of the family? To be so afraid and untrusting of the world that you don’t believe anyone actually wants to help? I don’t know what happened to both children after the transfer, but hope to find out by the end of the day.
I am beyond humbled by their plight. I am posting pictures, not to exploit their situation, but because I sincerely, passionately believe it is the only way we can see outside of our own bubbles. The pictures do far more justice to the situation than my words – all pictures posted are done so with permission from the affected patients or their guardians. They also expressed permission that that these images could be shared with others outside of Bangladesh.
These people really need our help, desperately. I hope that small acts of kindness can hopefully, collectively, bring about true and lasting changes for them. Naive as it may sound, I will always believe humanity must prevail.
January 15, 2018: Day 7, Thaingkhali Camp Block A
“Life’s most persistent and urgent question is, ‘What are you doing for others?’” ~Martin Luther King, Jr.
My response – no matter what I’m doing, it doesn’t seem to be enough.
After taking Sunday off, I returned to camp on Monday, the 15th, with Team 4 members from IMANA, who safely arrived yesterday in Bangladesh. The desolation of these camps is unreal. The circumstances surrounding these people are unfathomable, yet we walk through these barren hills every morning and witness life as it should never exist.
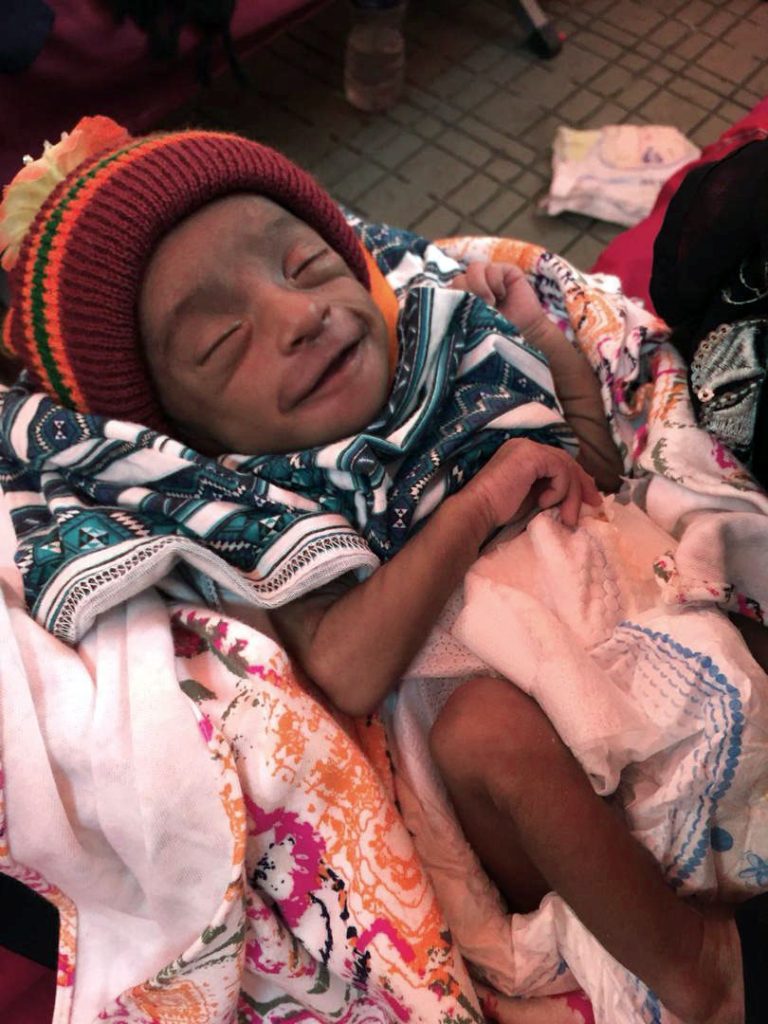
Miss Rashida 36 hrs after hospital stay
There was great news to start off the day – Lil’ Miss Rashida!!! From a frightening 1 kg weight at 38-days-old, she had already gained 1 lb (0.5kg) in just 36 hours of admission at the Malaysia Field Hospital. She was now smiling! Keep on chugging, little one!
The update on little Mr. Mahmud was not as uplifting as Miss Rashida. Sadly, I found out yesterday that although he was admitted Saturday night, the father, for all the reasons previously mentioned, signed him out against medical advice (inconceivable in pediatrics in the U.S.!!!). My heart sank further because he only got one dose of antibiotics and didn’t get any oral medications upon his departure (I know the doctors at the field hospital tried very hard, but their resources are limited as well, especially after hours).

Mr. Mahmud’s home visit
After the mobile clinic ended this afternoon, I asked one of the local volunteers to walk me back to Mahmud’s “home”. It was a 25 minute hike back to Block C to their shack. When I found the mother, she was initially upset and afraid that I was back. She was quickly reassured that I wouldn’t take her child away, but rather I had sought out the family to give Tylenol and oral antibiotics for Mahmud so that he would get relief from fever and maybe have a chance at clearing the pneumonia. He was still feverish at the “home” visit, still breathing fast, and still not moving air well. I am haunted by her words to me that day after I explained why I was so worried that they left the hospital on Friday without treatment:
“Well, if he dies, he’ll die. God must have willed it. This is our reality.”
How does one keep a straight face? I believe she was hiding her true emotions and concern as she didn’t trust me. As we talked, a small crowd had gathered around us. One of the local women barked something to the mother that suddenly softened her demeanor and made her receptive to my visit. She was still firm that they would not return to the hospital. I asked her why, but received no response. I didn’t press any further for fear that she would then reject my medication instructions. I so desperately wanted to ensure that Mahmud had drugs for fever control and some form of antibiotic coverage. I gave her instructions on how to give both medications and then asked her to administer the first dose of antibiotics in my presence. At the end, she grabbed my hand as I got up to leave and nodded her head once.
I then took my leave… It rips me apart that this sweet little boy isn’t getting the best treatment available to him, but I’m not sure what could have been done differently. Please, please remember him in your prayers.
As my guide, Ibrahim, and I made the 1.5 mile trek back to the clinic site for the day, I asked him what the other woman said to Mahmud’s mother that relaxed her, and he sheepishly said, “Ma’am, she told her she’s being a fool – that the fact you came looking for them is shocking but because you’re a female doctor, your maternal instincts must have brought you back here. She should not fight Allah.” I am no psychologist but it offered a small glimpse into the mindsets of these people and the emotional trauma that has become woven into their DNA.
As the day ended, we collected another entourage on the trek back to our van. The children were initially so shy but so cute! They were delightfully playful and their smiles filled my heart. It was a fresh reminder of the resilience of children, the tenacity of human spirits, and more importantly, why it’s so important for us to try and save an entire generation from becoming lost.
To be continued…
What can you do?
Monetary contributions and volunteers are always needed by IMANA and the numerous other NGOs listed below, that are on the ground in Bangladesh. In addition, Burma Task Force (BTF) is a coalition of 19 US and Canadian Muslim organizations, under the parent organization, Justice For All, a 501(c)(3) nonprofit, dedicated to advocating for the Rohingya and ending the genocide in Burma. BTF encourages you to contact your senators and representatives and urge them to pass the Bill To Promote Democracy and Human Rights in Burma and the Burma Act of 2017. For more information and a specific action plan visit Burma Task Force.
NGOs on the ground in Bangladesh:
Bangladesh Rural Advancement Committee (BRAC)
International Rescue Committee
Tasneem Hoque, MD was inspired to return to her ancestral home of Bangladesh out of a deep desire to help with the devastating plight of the Rohingya people. Tasneem completed her residency in pediatrics and her fellowship in pediatric cardiology at Columbia University Medical Center in New York City. Providing care and service to people is her passion, but she is also committed to serving her community through various charity works, humanitarian causes, and by inspiring youth to achieve their dreams. She is a founding board member for the Khan Foundation, a 501(c)(3) nonprofit organization geared at improving college access to low-income and underprivileged youth in New York City.
Keep supporting MuslimMatters for the sake of Allah
Alhamdulillah, we're at over 850 supporters. Help us get to 900 supporters this month. All it takes is a small gift from a reader like you to keep us going, for just $2 / month.
The Prophet (SAW) has taught us the best of deeds are those that done consistently, even if they are small. Click here to support MuslimMatters with a monthly donation of $2 per month. Set it and collect blessings from Allah (swt) for the khayr you're supporting without thinking about it.

The Forgotten Pilgrims: Honoring Those Exempted From Hajj

Connecting With Al-Fattah And Ash-Shakur This Dhul Hijjah

Deadly Attack At San Diego Mosque Sends Shockwaves

The APA Gave Him A Human Rights Award. Then They Cut His Microphone For Talking About Gaza.

Stoning The Jamarat: Naming The True Enemy

Op-Ed: Javed Ghamidi And The Theology Of Managed Defeat

Why Liberation Is Sexual(ized) – The Forces Driving The Unquenchable Thirst To Emancipate Muslim Women

The APA Gave Him A Human Rights Award. Then They Cut His Microphone For Talking About Gaza.

Daughter Of Which Nation? The Persecution Of Asiya Andrabi And India’s Crackdown On Muslims

Beyond Representation: Reclaiming Spiritual Storytelling For Muslim Children

Coming Full Circle: Who Are You Now? | Night 30 with the Qur’an

Running Away From Who We Are | Night 29 with the Qur’an

Building From the Ground Up: Week 4 Recap | Night 28 with the Qur’an

The Muslim You Are Becoming | Night 27 with the Qur’an

What Will You Leave Behind? Legacy in Islam | Night 25 with the Qur’an
Trending
-
#Current Affairs3 weeks ago
Op-Ed: Javed Ghamidi And The Theology Of Managed Defeat
-
#Current Affairs3 weeks ago
Why Liberation Is Sexual(ized) – The Forces Driving The Unquenchable Thirst To Emancipate Muslim Women
-
#Current Affairs2 days ago
The APA Gave Him A Human Rights Award. Then They Cut His Microphone For Talking About Gaza.
-
#Society1 month ago
For Muslims In The US, Recognition Does Not Guarantee Safety














Usman
March 13, 2018 at 7:39 AM
Wow, what a mix of thoughts and emotions I have after reading that piece! Allah bless this doctor for her selfless service and may Allah ease the suffering of these unfortunate people. Seeing people suffer just because they were born into a certain race or region of the world makes me think about the injustices of life. And my own ungratefulness for the blessings I have irrespective of postmodern western stresses of debt, taxes, inadequate health insurance, missed mortgage payments, and other mundane matters. There is two thought pathways that are elicited after reading about such horrific atrocities. The first is that it’s just these people’s bad luck in an atheistic worldview. The second thought is that there is a God and universal justice. My cognitive conclusion is the latter with the understanding that the afterlife will provide compensation for their suffering. Allah knows best…
Simeen
March 18, 2018 at 11:48 AM
Barakallahu feekum. Jazakillahu khayran for sharing.
Abdul Rahman
April 3, 2018 at 10:19 AM
gud wrk……jzk. i pray they receive all the help they need from the ummah